Oral ulcers are painful, often recurrent lesions that develop in the soft tissues of the mouth, including the inner cheeks, lips, tongue, floor of the mouth, and soft palate. These ulcers can vary in size, shape, and severity, and may result from a variety of causes, including trauma, infection, systemic conditions, or idiopathic factors. Understanding the common types of oral ulcers is crucial for proper diagnosis, management, and prevention.
Aphthous Ulcers (Canker Sores)
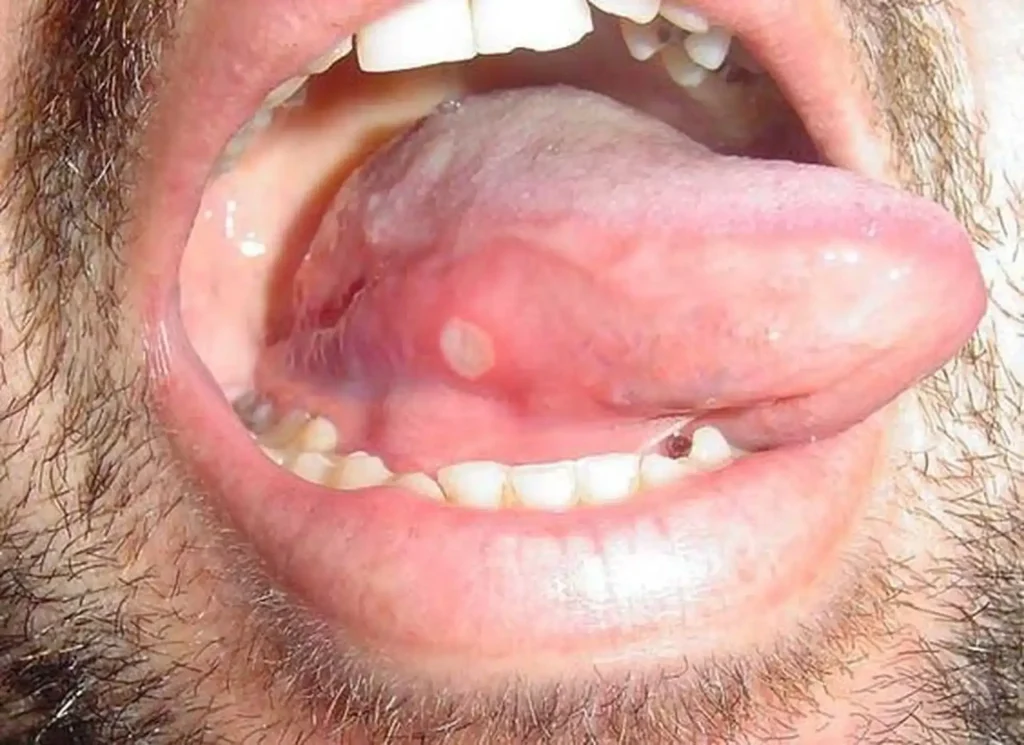
Aphthous ulcers are the most frequent type of oral ulcers, affecting up to 20% of the general population. They are small, round or oval lesions with a yellow or white center and a red halo. These ulcers are painful and appear on non-keratinized mucosa, such as the inside of the cheeks, lips, or under the tongue. There are three clinical types:
- Minor aphthous ulcers (most common): Less than 1 cm in diameter, heal within 1–2 weeks without scarring.
- Major aphthous ulcers: Larger than 1 cm, may take weeks to heal, and can leave scars.
- Herpetiform ulcers: Multiple small ulcers (1–3 mm), often clustered, may resemble herpes but are not caused by the herpes virus.
The exact cause of aphthous ulcers is unknown; however, potential triggers include stress, nutritional deficiencies (especially iron, vitamin B12, and folic acid), hormonal changes, and certain food sensitivities.
Traumatic Ulcers
Traumatic ulcers result from physical injury to the oral mucosa. Common causes include accidental cheek biting, irritation from sharp teeth, ill-fitting dentures, or aggressive tooth brushing. These ulcers are painful and usually singular, appearing at the site of trauma. Once the source of irritation is removed, they typically heal within 7–10 days.
Herpes Simplex Virus (HSV) Ulcers
Primary infection with HSV, usually HSV-1, can cause acute herpetic gingivostomatitis, especially in children. This condition presents with multiple painful ulcers on the lips, gums, and inside the mouth, accompanied by fever and swollen lymph nodes. After the initial episode, the virus remains dormant and can reactivate, often presenting as recurrent cold sores on the lips or perioral skin.
Oral Ulcers in Systemic Diseases
Certain systemic conditions can manifest as oral ulcers:
- Behçet’s disease: Recurrent oral and genital ulcers with systemic involvement.
- Tuberculosis: Painless ulcer on lip, cheek, tongue, or palate, originating from primary or secondary pulmonary tuberculosis.
- Syphilis: Primary or secondary syphilis can manifest into painless oral ulcers, maybe single or multiple, lasting for 4-6 weeks.
- Lupus erythematosus: May cause chronic oral ulcers, especially on the palate.
- Inflammatory bowel diseases (e.g., Crohn’s disease, ulcerative colitis): May lead to oral lesions.
- HIV/AIDS: Often associated with chronic and multiple oral ulcers due to immunosuppression.
Drug-Induced Ulcers
Some medications, such as NSAIDs, chemotherapeutic agents, and beta-blockers, can cause oral ulcers as side effects. These ulcers usually resolve upon discontinuation or adjustment of the medication.
Malignant Ulcers
Malignant ulcer or oral cancer is critical from the perspective of the rural population in our country. It is painless but rapidly growing, destroying all kinds of tissues, including the bone. Smoking and chewing habits are the prime causes of oral malignant ulcers. Early diagnosis and prompt treatment are crucial to cure this ulcer and save the life.
Conclusion
Oral ulcers are common and usually benign, but persistent, large, or recurrent lesions warrant clinical evaluation to rule out underlying systemic conditions or malignancy. In cases of uncertainty, biopsy and laboratory testing may be necessary for definitive diagnosis. Proper oral hygiene, balanced nutrition, and avoidance of known triggers can help prevent and manage oral ulcers.